Faculty call for end to pelvis classification system in new paper
Paper featured in special issue of The Anatomical Record Heading link

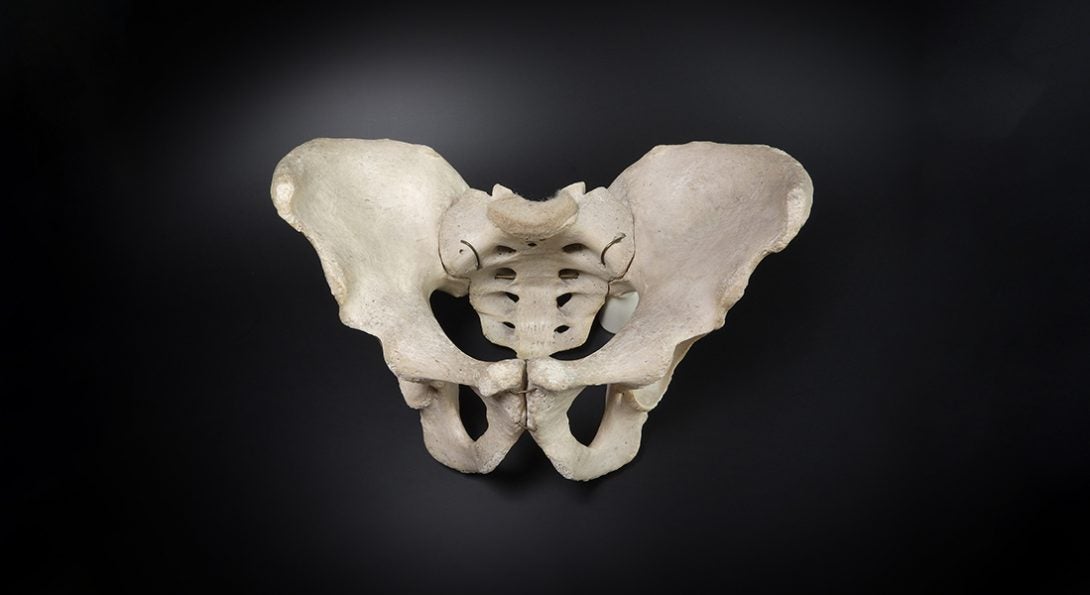
A female pelvis classification system that was first developed in the 1930s and is still widely used in obstetric and midwifery books should be abandoned, argue two UIC College of Nursing faculty in a new paper published in the journal The Anatomical Record.
UIC Nursing associate professor Julienne Rutherford, PhD, and assistant professor Kylea Liese, PhD, CNM, are co-authors on the paper. Caroline VanSickle, PhD, an assistant professor at A.T. Still University, is lead author.
The paper is featured in a special issue of the journal The Anatomical Record focused on the changing face of the discipline of anatomy.
The authors call upon instructors to stop teaching the Caldwell-Moloy classification system of the female pelvis shape. They ask that textbook editors remove the system from books and argue that the material should also be taken off certifications and board exams.
“The original study would not pass peer review today,” VanSickle says. “It used cherry-picked data to support [Caldwell and Moloy’s] preconceived notion of what they thought they were seeing in the clinic as obstetricians at the time and did not include a rigorous test of any sort of hypothesis.”
The Caldwell-Moloy system was developed by two physicians in the 1930s and defines four primary types of the female bony pelvis, linking each with a different birth outcome. Their goal was to develop a method that allowed obstetricians to identify patients who might have difficulty in childbirth because of the normal shape of their bony pelvis, and to use that knowledge to apply clinical interventions, such as surgery or forceps.
“What is missing from these textbooks and from Caldwell and Moloy’s original study is evidence demonstrating a correlation between pelvic inlet size and shape and particular birth outcomes; in fact, such evidence remains elusive today,” the authors write.
The system does not account for the many other factors that lead to birthing difficulty and overestimates the impact of pelvis shape on birth, according to the paper.
Liese, who is a midwife, says when pregnant patients are admitted to the hospital for labor, many practitioners still indicate whether the patient has an “adequate pelvis” in the electronic medical record.
“Women have been denied opportunity for a vaginal birth because they were told their pelvis shape was not conducive to it without real evidence to support that determination,” she says.
The authors also explain that the system perpetuates racism in maternal healthcare, resulting in health disparities. The data used to support Caldwell and Moloy’s system was based on “racist underpinnings,” the authors write, which have contributed to stereotypes, such as the persistent assumption that childbirth is easier and less painful for Black women.
Rutherford, who teaches anatomy to midwifery students, says as of fall 2021, she removed the classification system from the graded portion of her class.
“The way we teach this content is how it gets there into the public,” she says. “It’s how pregnant people talk to each other, how it shapes anxieties and expectations about pregnancy, and their experience with childbirth. We have a responsibility to change that narrative.”